Migraine Attacks Independent of CGRP (cGMP-mediated migraine)
Posted on June 09 2024,
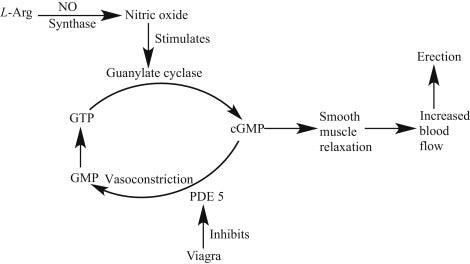
A randomized, double-blind, placebo-controlled study published in Cephalalgia investigated whether sildenafil (Viagra), a phosphodiesterase-5 (PDE-5) inhibitor that increases cGMP levels, could induce migraine attacks in individuals with migraine who were pre-treated with erenumab (Aimovig), a calcitonin gene-related peptide (CGRP) receptor monoclonal antibody.
The study found that 63% of participants experienced a migraine attack within 12 hours after taking sildenafil, compared to only 19% after taking placebo. These findings suggest that the cGMP pathway can trigger migraine attacks INDEPENDENTLY of CGRP receptor activation.
The clinical implications of this study are significant. First, it emphasizes that migraine pathophysiology is complex and involves multiple signaling pathways. Second, it highlights the cGMP pathway as a potential target for future migraine treatments, particularly for patients who do not respond adequately to CGRP-targeted therapies or experience side effects from these treatments.
The study also raises the possibility of developing personalized migraine treatments based on an individual's predominant migraine-triggering pathways. Patients with migraine primarily driven by the cGMP pathway might benefit more from therapies targeting this pathway, while those with CGRP-driven migraine might respond better to CGRP-targeted treatments. Furthermore, combination therapies targeting both pathways simultaneously might provide increased efficacy for some patients (this is currently being studied with anti-PACAP and anti-CGRP drugs).
While the specific mechanisms by which cGMP contributes to migraine pathogenesis remain to be fully known it may be easy to jump to the conclusion that it is vasodilation due to the mechanism of action and clinical outcome of sildenafil. However, the study's authors discuss potential sites of action of sildenafil within the trigeminovascular system. They note that sildenafil, being a lipophilic drug, can cross the blood-brain barrier and exert central effects, potentially activating excitatory neuronal pathways that may contribute to migraine attack initiation. Remember, migraine is neurovascular, not solely vascular in pathogenesis.
It is important to note that this study is small and further research is needed to confirm these findings and fully understand the clinical implications of targeting the cGMP pathway in migraine management.
Candesartan for Migraine Prevention: What New Research Shows
New 2026 research shows candesartan, a low-cost blood pressure pill, can prevent migraines. Here is what the evidence says about how ARBs work, dosing, safety, and who should consider them.
Read MoreFri, May 08, 26
Does the Side of Your Migraine Actually Matter?
If you've been told your migraine attacks are damaging your brain or that the side they're on predicts anxiety or PTSD, the evidence doesn't support it.
Read MoreMigraine, Menopause, and Hormonal Health
Migraine affects women three times more than men, and menopause does not always bring relief. Nearly half of women continue having migraine attacks after menopause. Learn what the research says...
Read More




